The Importance of Clinical Correlation: A Real Case Showing Why MRI Reports Must Be Interpreted Carefully
When patients suffer spinal injuries after a motor vehicle collision, MRI is often viewed as the “gold standard” for diagnosis. But even the most advanced imaging is only as useful as the interpretation behind it. A recent case in our office highlighted the importance of clinical correlation, precise imaging review, and interprofessional collaboration between chiropractors, pain management physicians, and neurosurgeons.
This case demonstrates how an inaccurate radiology report can delay care, how proper clinical examination clarifies the diagnosis, and how coordinated communication leads to appropriate treatment and recovery.
The Patient’s Initial Findings
The patient presented with lower back pain and neurological symptoms after an injury. Standard lumbar MRI imaging was performed, and the radiologist reported disc desiccation, circumferential bulging, facet arthropathy, and moderate bilateral foraminal stenosis at L5–S1, but made no mention of a herniation.
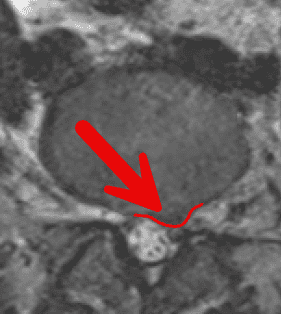
However, the MRI images clearly revealed a different story.
In the sagittal and axial views on page 4 of the case report there is unmistakable evidence of a left paracentral focal lesion, consistent with a disc herniation affecting the left L5 nerve root. The lesion is broader at the base and narrower at the apex, confirming a protrusion-type herniated disc, not merely a disc bulge.
This discrepancy between the radiologist’s report and the actual imaging findings created significant risk for misdiagnosis and undertreatment.
Why This Matters: Clinical Exam + Imaging = Accuracy
MRI is extremely valuable, but it must always be interpreted alongside:
Sensory testing
Motor strength evaluation
Deep tendon reflexes
Dermatomal distribution of symptoms
Your case report notes that many clinicians rely only on patellar and Achilles reflexes, which leaves major diagnostic gaps when correlating L5 nerve root involvement. In this case, the combination of clinical exam findings and personal review of MRI imaging clarified the true source of the patient’s symptoms.
This is why clinical correlation is not just recommended—it is mandatory for accurate diagnoses.
Correct Diagnosis Changed the Entire Treatment Plan
Once the disc herniation was correctly identified, the patient was referred to interventional pain management. A left-sided L5/S1 epidural steroid injection was performed, and she initially experienced relief in the recovery room.
However, when the anesthetic wore off, the patient began experiencing significant left lower extremity pain, indicating that the disc herniation was more severe than originally understood.
Because the correct diagnosis had been established and coordinated communication was already in place, a neurosurgical consultation was arranged immediately. When the patient’s condition worsened, she was met in the Emergency Department and underwent an urgent L5/S1 microdiscectomy.
This would not have occurred if the original radiology report had been followed without question.
The Lesson: Imaging Is Only One Piece of the Puzzle
This case reinforces several important points for patients and providers:
1. Radiology reports can be incomplete or inaccurate.
Radiologists do not examine the patient. They interpret what they see—but sometimes key findings are missed, mislabeled, or understated.
2. Clinical correlation changes everything.
A herniation is not just an imaging finding. It has real neurological consequences. Matching imaging to symptoms is what leads to correct decisions.
3. Accurate diagnosis requires collaboration.
In this case, communication between a chiropractic physician, pain management specialist, neurosurgeon, and the patient ensured:
the correct injury was identified
the right specialist was involved
the patient received appropriate, timely care
This is exactly how integrated care should function.
What This Means for Patients and Attorneys
For patients:
You deserve providers who examine you thoroughly, review your imaging with precision, and communicate with your full team. Accurate diagnosis leads to better outcomes.
For attorneys:
Medically defensible documentation requires more than accepting radiology reports at face value. Expertise in reading MRI studies ensures your clients’ injuries are correctly identified and treated.
For clinicians:
This case underscores the importance of confirming radiology impressions with your own diagnostic reasoning.
Our Approach at Eatontown Elite Care Center
As a Fellowship-trained Primary Spine Care provider, I emphasize:
Advanced imaging interpretation
Neurological correlation
Evidence-based care pathways
Timely referral when appropriate
Direct communication with medical and legal stakeholders
Cases like this reaffirm our mission: deliver accurate diagnoses, protect patients from mismanagement, and ensure they receive the care they truly need.